In cases of tooth loss, dental implants are the best alternative when a sufficiently durable, aesthetically pleasing, and effective tooth replacement is needed. However, this method cannot be used for everyone; for example, diabetics require greater attention.
It is important to highlight right from the start that diabetes and implants are not mutually exclusive, however, due to the higher risk in diabetic patients, such a procedure requires consideration of several aspects.
But why is this the case? What are the health risks of implantation in the case of diabetes, why is it important to pay attention to the HbA1c level, and what is the professional opinion on the matter? We have gathered all the important information in our article!
Mi is az a fogászati implantátum?
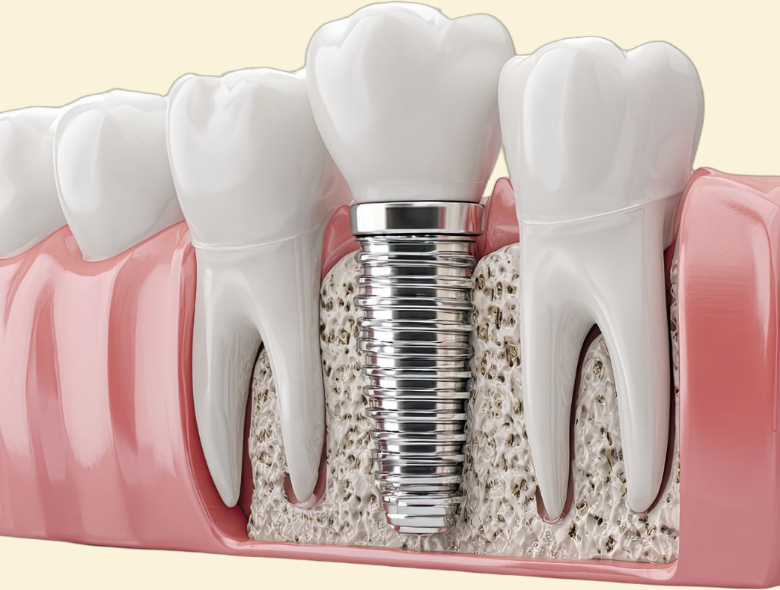
To understand why dental implants are riskier for a diabetic patient, we first need to be aware of the main characteristics of this tooth restoration method.
In brief, implants are artificial tooth roots, mostly made of titanium, which are surgically attached directly to the jawbone or gums.
The implantation is followed by a healing process that often lasts for months, during which the implant must fuse closely with the jawbone tissue, meaning it must integrate with the body.
This is a demanding, yet mostly risk-free process for a healthy person; however, healing can be much more complicated for those with diabetes.
The health risks of diabetes in case of an implant
Diabetes is one of the most common metabolic diseases, which impairs the body's natural ability to process sugar. Insulin, produced by the pancreas, is responsible for breaking down sugar.
If insulin production is disrupted for any reason and its quantity decreases in the body, it can lead to numerous health problems, causing blindness, nerve damage, and even kidney disease if left untreated.
The dental risks of diabetes
However, it should be known that diabetes also carries many risks from a dental perspective. Observations and research, for example, confirm that individuals with diabetes are much more likely to develop gum disease that leads to tooth loss.
It is very important to be aware of this before implant placement, as whether the tooth implant is carried out due to diabetes complications or for other reasons, healthy gums are essential for this.
Risks of post-implantation recovery
Provided that someone has diabetes but receives appropriate treatment and maintains good oral hygiene, they can undergo implantation, however, complications may still arise after the procedure.
The biggest problem for diabetics is the risk of infection. In their case, there is a much higher chance of infections developing compared to healthy patients.
The reason for this lies in the disease's ability to slow down, or even hinder, the body's resistance to infections. Gum disease can be traced back to this, as can the infection of an implant after a dental implant procedure.
Furthermore, in diabetics, healing is often much slower, and there can even be cases where implants do not become infected but also cannot bond with the bone tissue, meaning dental crowns cannot be placed on them.
Diabetics can also receive dental implants!
Despite the above risks, it is very important to highlight that diabetics can also receive dental implants – regardless of whether they suffer from type 1 or type 2 diabetes.
The condition for this is good health and proper oral hygiene, along with continuously managing their condition and keeping blood sugar levels under control.
Whether a diabetic patient is suitable for implantation is primarily determined by their HbA1c level. Here are the most important things to know regarding this!
HbA1c levels and dental implantation in diabetics
The determination of glycated haemoglobin, or HbA1c level, is necessary before implant placement in a diabetic patient because this value determines the average blood sugar level for the past 2-3 months and also informs the dentist about the quality of glycemic control.
These are very important values because only through scientific methods can it be ascertained that the patient is indeed keeping their blood sugar level under control, which otherwise can be a disqualifying factor for implant placement.
There are several methods for determining HbA1c levels. The most accurate and most accessible is the traditional blood test, which can determine the value from blood taken from a vein in the arm, under laboratory conditions.
In addition, there are now rapid tests available that can show a patient's HbA1c level from just a few drops of capillary blood.
Implantation is safe with an adequate HbA1c level
Research confirms that patients suffering from diabetes may have up to a 50 percent higher incidence of developing inflammation following implant placement compared to healthy individuals.
Particular attention must be paid to the HbA1c level. If these values are appropriate, meaning the patient has carefully managed diabetes, then the success rate of dental implant placement can exceed 92 percent.
This means that the procedure is only minimally more risky than for healthy patients and bone healing is expected to proceed properly, although the healing time may increase.
Naturally, individual assessment is necessary for every patient. Furthermore, the application of extra treatments cannot be ruled out, so for example, the chances of implant survival and healing can be improved with antibiotic treatments and special mouthwashes.
The ideal HbA1c level for implant placement
It is therefore already clear that measuring HbA1c levels is essential for the success of implantations in diabetic patients, but what is the normal value for this, and how often is it necessary to check the level?
The American and European Diabetes Associations both agree that if a person has a normal HbA1c level, it only needs to be repeated twice a year, but in other cases, it must be checked quarterly before implantation.
The ideal HbA1c level according to the two societies is 7 percent, which is a maximum of 53 mmol/mol in the case of traditional blood sampling.
The lower this ratio is in a diabetic patient, the greater the chance of reducing the risk of complications associated with implant placement.
Furthermore, there is an 8% target that has been set for patients who have a limited life expectancy or for whom overly strict glycaemic control would do more harm than good.
Therefore, in their case, the implant can be placed even with a somewhat higher HbA1c level, but the patient-dependent nature of the target values cannot be emphasised enough, as age, pregnancy, general health condition, and even haemoglobin disorders can determine it.
In the case of a diabetic patient, the possibility of implant placement is always subject to individual assessment, and the glycated haemoglobin measure is just one of the most important factors that must be taken into account in such cases.
The opinion of dental associations regarding diabetes and implants
It has thus become apparent from the above that, according to diabetes associations and societies, a HbA1c value of 7-8 percent does not preclude diabetes as a contraindication if a patient wishes to have an implant.
However, it is also worth examining the position of dental associations on the subject, as both the American Academy of Periodontology and the European Federation of Periodontology have expressed a firm opinion, dedicating a separate chapter to the subject.
The two associations have divided patients suffering from diabetes into categories. In light of this:
Diabetics with an HbA1c level below 7 percent are classified in category B, meaning implantation is not a problem for them.
Diabetics with an HbA1c value above 7 per cent are classified as category C, and implantation is no longer recommended for them.
Even more interesting is the position of the German Society of Dental and Oral Medicine (DGZMK) and the German Association for Implantology (DGI) on the subject, who divide diabetic patients into three groups. In their case, the classification is as follows:
An HbA1c value between 6-8%: appropriately managed diabetes, which does not preclude the implantation of an implant.
An HbA1c value between 8-10%: moderately controlled diabetes, which, with appropriate treatment, does not yet preclude the use of an implant.
An HbA1c value above 10%: poorly controlled diabetes, which in all cases excludes implant placement.
Frequently asked questions
What extra preparation does a diabetic patient require for implant placement?
It is extremely important for a diabetic patient to consult with their treating physician – preferably an endocrinologist – before implant placement, and to do everything possible to stabilise their blood sugar levels.
Furthermore, establishing and maintaining proper oral hygiene is essential, which can be preceded by targeted dental treatments, such as tartar removal.
Which type of implant is recommended for diabetics?
There isn't an implant specifically developed for diabetics, but due to their biocompatible nature, titanium implants are more fortunate, as they heal more easily and ossify faster than other types.
Does a diabetic need to go for more frequent check-ups after an implant?
Absolutely, as diabetes can slow down the healing process, initially even monthly check-ups may be necessary, and later annual routine examinations are equally important. The implantologist specialist will provide precise information on this in every case.
Are there alternatives to implants for diabetics?
In modern dentistry, numerous options are now available for dental prosthetics for diabetics. If the adjacent teeth are suitable, a dental bridge can be a good alternative, but for multiple missing teeth, both a partial or a full denture are suitable decisions.
Can blood sugar levels rise after implant surgery?
While not typical, it is normal for blood sugar levels to increase slightly due to the stress caused by surgical intervention, so it is advisable to measure more frequently and consult with an endocrinologist.
Is an antibiotic course necessary for a diabetic patient following implant placement?
As the risk of infection is higher, a course of antibiotics is often necessary for healing to commence under the right conditions.
Can diabetes that develops after implant placement cause risks?
If someone pays attention to their oral hygiene, controls their blood sugar levels, and regularly attends dental check-ups, then the level of risk or the probability of developing complications is very minimal.